Key Takeaways
- •Fungal acne (pityrosporum folliculitis) is caused by yeast, not bacteria — so antibacterial acne treatments won't work.
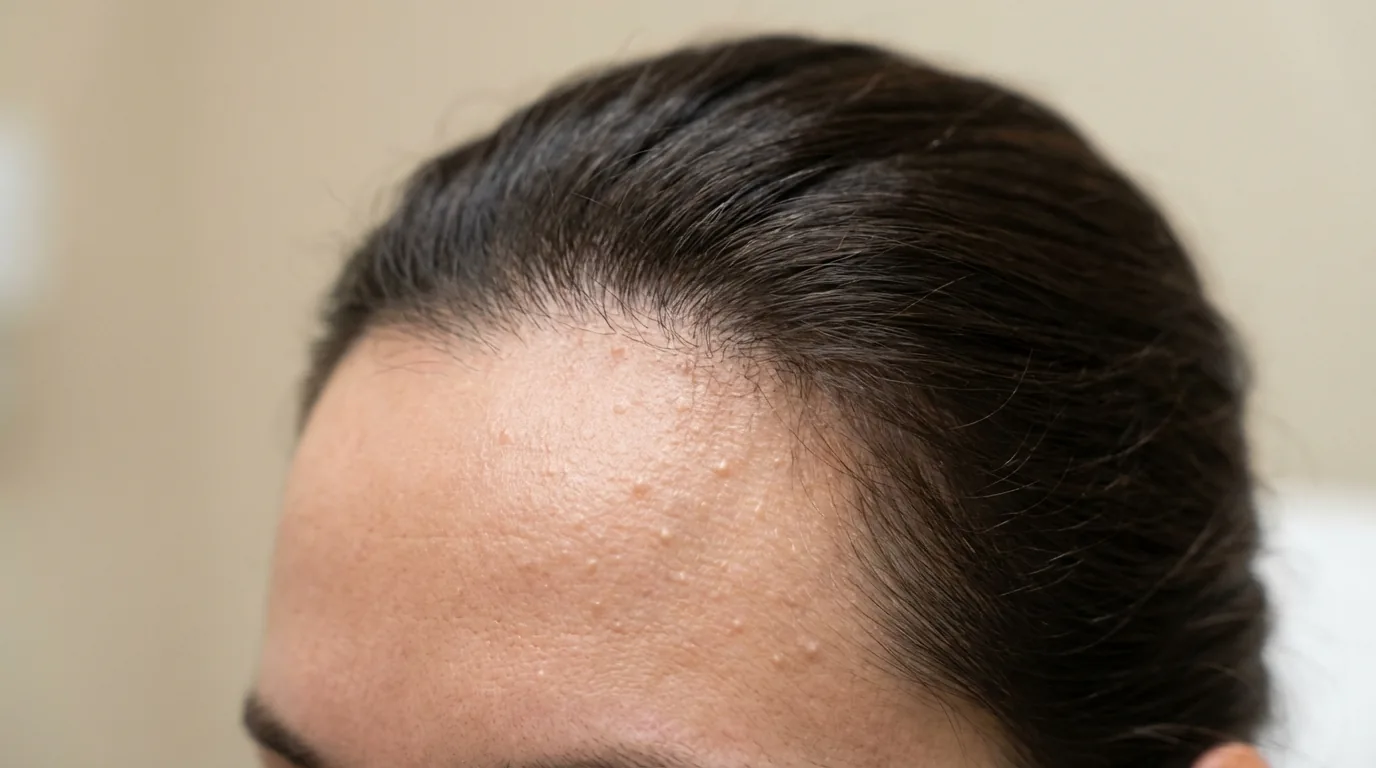
- •It presents as uniform, itchy, small bumps typically on the forehead, chest, and back.
- •Oral antibiotics can actually worsen fungal acne by disrupting the skin's microbial balance.
- •Antifungal treatments — both topical and oral — are the primary solution.
- •Many common skincare ingredients feed the yeast that causes fungal acne.
- •Proper diagnosis requires distinguishing it from bacterial acne, closed comedones, and keratosis pilaris.
What Fungal Acne Really Is
Fungal acne is the colloquial term for pityrosporum folliculitis (also called Malassezia folliculitis), an inflammatory condition caused by an overgrowth of Malassezia yeast within the hair follicle. Despite sharing the word 'acne' in its common name, it is not acne vulgaris and has a completely different pathophysiology. Acne vulgaris is driven by Cutibacterium acnes bacteria, excess sebum, and abnormal follicular keratinization. Fungal acne is an infection of the follicle by commensal yeast.
Malassezia is a genus of lipophilic yeasts that are part of the normal human skin flora — they live on everyone's skin. Problems arise when conditions shift in their favor, allowing overgrowth. Factors that promote Malassezia overgrowth include hot, humid environments, excessive sweating, occlusive clothing, immunosuppression, and the use of broad-spectrum antibiotics that reduce competing bacteria.
Understanding this distinction is critical because it explains why conventional acne treatments fail and can even worsen the condition. Benzoyl peroxide targets bacteria, not yeast. Oral antibiotics kill competing bacteria, giving Malassezia more room to proliferate. Many acne-targeted moisturizers and oils contain fatty acids and esters that literally feed the yeast.
How to Identify Fungal Acne
The hallmark of fungal acne is uniformity. While bacterial acne presents as a mix of different lesion types — blackheads, whiteheads, papules, pustules, and cysts of varying sizes — fungal acne appears as monomorphic (same-sized) papules and pustules, typically 1–2mm in diameter. They often appear in crops or clusters rather than as scattered individual lesions.
Location is another key differentiator. Fungal acne favors the forehead, chest, upper back, and shoulders — areas with high sebaceous gland density and increased sweating. It's less common on the lower face and jawline, which are classic locations for hormonal bacterial acne. The lesions are frequently itchy, which is unusual for true acne — most bacterial acne lesions are painful or tender rather than pruritic.
The clinical history often provides important clues. Fungal acne frequently develops after a course of oral antibiotics, during hot and humid weather, or in individuals who exercise heavily without immediately showering. It often doesn't respond to — or worsens with — standard acne treatments including benzoyl peroxide, topical retinoids, and oral antibiotics.
Why Standard Acne Treatments Fail
The failure of standard acne treatments is actually one of the most useful diagnostic features of fungal acne. If you've tried benzoyl peroxide, salicylic acid, topical retinoids, and even oral antibiotics without improvement — or with worsening — fungal acne should be high on the differential diagnosis.
Oral antibiotics deserve special mention because they can directly cause fungal acne. Tetracyclines (doxycycline, minocycline) and other broad-spectrum antibiotics suppress the bacterial component of the skin microbiome, removing the competitive inhibition that normally keeps Malassezia in check. This is why fungal acne frequently develops during or after antibiotic courses intended to treat bacterial acne.
Many popular skincare products also contribute to the problem. Malassezia thrives on specific fatty acids and esters that are common in moisturizers, sunscreens, and makeup. Fatty acids with carbon chain lengths of 11–24 (with the exception of capric and caprylic acid) feed the yeast. Common culprits include isopropyl palmitate, isopropyl myristate, lauric acid, and many plant oils including coconut oil and olive oil.
Effective Treatment Strategies
The cornerstone of fungal acne treatment is antifungal therapy. For mild to moderate cases, topical antifungals are often sufficient. One of the most well-known accessible treatments in the skincare community is Nizoral A-D Anti-Dandruff Shampoo. Despite being a hair product, its active ingredient ketoconazole is a proven antifungal that works directly on Malassezia. The method is straightforward — apply a small amount to the affected area, leave it on for a few minutes, then rinse. Many people see noticeable improvement within two to three weeks of consistent use.
For a complementary approach, The Inkey List Beta Hydroxy Acid provides salicylic acid that helps clear the follicles of debris without feeding the yeast, as salicylic acid is one of the few common acne ingredients that doesn't worsen fungal acne. It works by penetrating into the follicle to dissolve the buildup that traps yeast.
For moderate to severe or resistant cases, oral antifungals may be necessary. Fluconazole (150–200mg weekly for 2–4 weeks) or itraconazole (200mg daily for 1–2 weeks) are the most commonly prescribed options. Oral treatment is particularly valuable because it addresses the Malassezia systemically, reaching follicles that topical treatments may not penetrate adequately.
Building a Fungal Acne-Safe Routine
Beyond active antifungal treatment, your entire skincare routine needs to be fungal acne-safe — meaning free of ingredients that feed Malassezia. This requires careful label reading, as many products marketed for acne-prone skin contain problematic ingredients. The key is avoiding fatty acids with chain lengths of C11–C24, esters of those fatty acids, and fermented ingredients.
Safe moisturizing options include Vanicream Moisturizing Skin Cream, which has a minimal, Malassezia-safe ingredient list and provides effective barrier support without feeding yeast. Squalane oil (derived from olives or sugarcane) is another safe option — it's a hydrocarbon, not a fatty acid, so Malassezia cannot metabolize it.
For cleansing, sulfur-based or zinc pyrithione cleansers are ideal choices because they have intrinsic antifungal properties. Avoid oil-based cleansers and heavy micellar waters. For sunscreen, mineral formulations with zinc oxide and titanium dioxide are generally safer than chemical sunscreens, which often contain problematic esters as the vehicle.
Preventing Recurrence
Fungal acne has a high recurrence rate because Malassezia is a commensal organism — it's always present on the skin and ready to overgrow when conditions permit. Prevention strategies focus on keeping the yeast population in check and minimizing conditions that favor overgrowth.
If you're prone to fungal acne, incorporate maintenance antifungal treatment into your routine. Using a ketoconazole shampoo as a body wash once or twice weekly can help prevent recurrence. Changing out of sweaty clothes promptly after exercise, showering as soon as possible after heavy sweating, and wearing breathable fabrics all reduce the warm, moist environment that Malassezia prefers.
Be cautious about reintroducing products that contain Malassezia-feeding ingredients. Once your fungal acne has resolved, you might be tempted to return to your old favorites, but if the yeast overgrowth was triggered by those products in the first place, it will likely recur. Building a permanent fungal acne-safe routine is the most reliable long-term prevention strategy.
When to See a Dermatologist
While mild fungal acne can often be self-treated with over-the-counter antifungals, certain situations warrant professional evaluation. If you've been using ketoconazole or other topical antifungals consistently for 4–6 weeks without improvement, a dermatologist can confirm the diagnosis — sometimes through a simple skin scraping and KOH preparation that visualizes the yeast under a microscope.
Dermatologists can also distinguish fungal acne from other conditions that mimic it, including bacterial folliculitis, closed comedones, keratosis pilaris, and gram-negative folliculitis. Each of these requires different treatment, and misdiagnosis leads to prolonged frustration and wasted effort.
If oral antifungals are needed, a dermatologist can prescribe the appropriate medication and monitor for side effects, particularly liver function with longer courses of azole antifungals. They can also investigate underlying factors that may be promoting recurrent Malassezia overgrowth, such as immunosuppression or hormonal imbalances.
References
- Rubenstein RM, Malerich SA. "Malassezia (Pityrosporum) folliculitis." Journal of Clinical and Aesthetic Dermatology. 2014;7(3):37-41.
- Saunte DML, et al. "Malassezia-associated skin diseases, the use of diagnostics and treatment." Frontiers in Cellular and Infection Microbiology. 2020;10:112.
- Prohic A, et al. "Malassezia species in healthy skin and in dermatological conditions." International Journal of Dermatology. 2016;55(5):494-504.