Key Takeaways
- •Keratosis pilaris (KP) affects up to 40% of adults and 50-80% of adolescents.
- •It's caused by excess keratin plugging hair follicles, not by poor hygiene or diet.
- •KP is genetic and cannot be cured, but it can be managed effectively with the right routine.
- •Chemical exfoliants (AHAs and urea) are more effective than physical scrubs.
- •Consistent moisturizing is just as important as exfoliation for managing KP.
- •KP often improves naturally with age and tends to be worse in winter.
Understanding Keratosis Pilaris
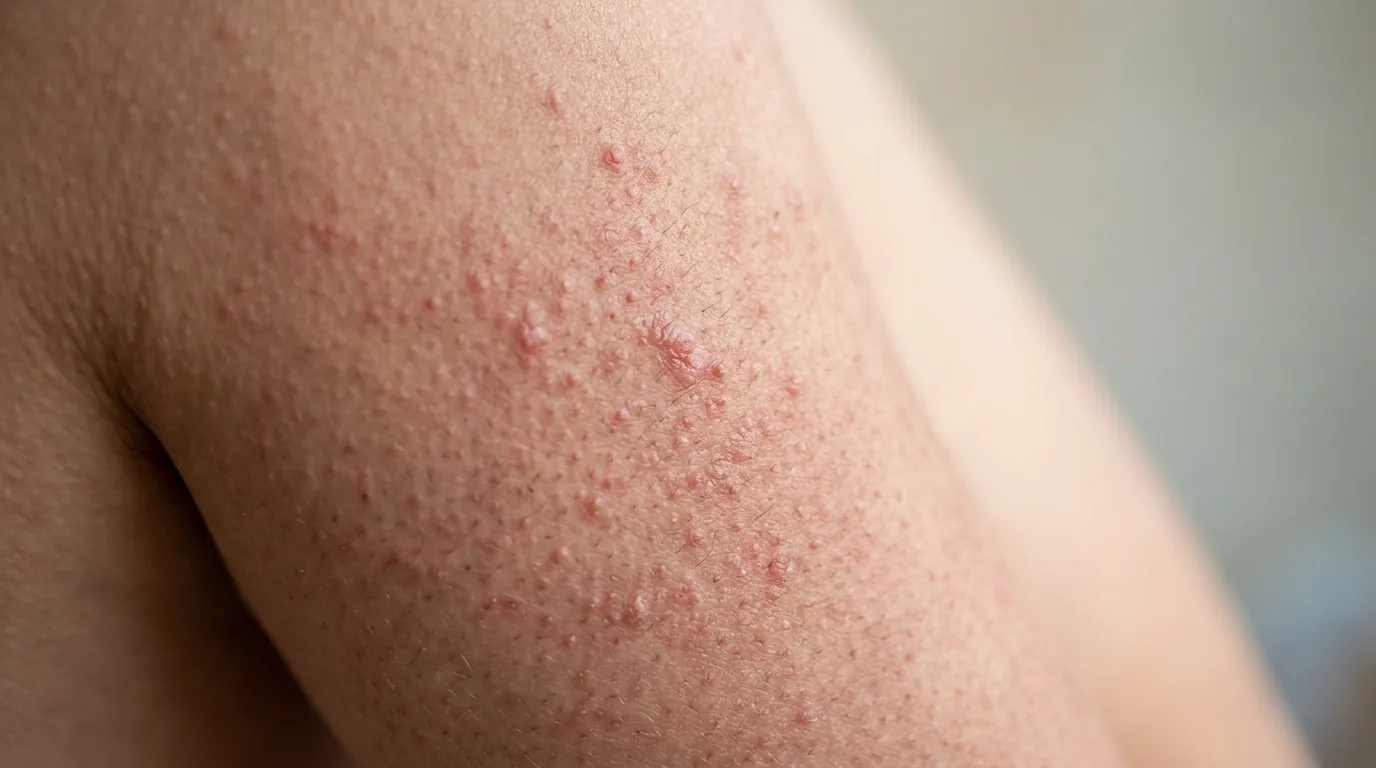
Keratosis pilaris (KP) is one of the most common skin conditions in the world, affecting an estimated 40% of adults and up to 80% of adolescents. Despite its prevalence, it's widely misunderstood — many people don't know what the condition is called, let alone what causes it or how to treat it. The characteristic rough, bumpy texture on the upper arms, thighs, buttocks, and sometimes cheeks is often mistaken for acne, dry skin, or an allergic reaction.
At its core, KP is a disorder of keratinization — the process by which skin cells produce and shed keratin, the structural protein that makes up the outer layer of skin. In KP, excess keratin accumulates around individual hair follicles, forming small plugs that trap the hair beneath the surface. These plugs create the characteristic rough papules that give the skin its 'chicken skin' or 'goosebump' texture.
KP is a genetic condition with autosomal dominant inheritance, meaning if one parent has it, there's approximately a 50% chance their children will too. It's associated with other atopic conditions — eczema, asthma, and allergic rhinitis — and individuals with these conditions are more likely to have KP. The condition is not caused by poor hygiene, dietary choices, or anything within your control.
Why KP Gets Worse in Winter
If you've noticed your KP worsening during cold months and improving in summer, you're not imagining it. Low humidity environments cause increased transepidermal water loss, leading to drier skin that's more prone to excessive keratinization. The keratin plugs become more prominent and visible when the surrounding skin is dehydrated.
Indoor heating compounds the problem by further reducing ambient humidity. The combination of cold, dry outdoor air and heated indoor environments creates conditions that exacerbate KP significantly. This seasonal pattern is so consistent that many people with KP describe their condition as having a clear winter-summer cycle.
Conversely, summer humidity, sun exposure, and increased sweating all tend to soften keratin plugs and improve the skin's texture. UV exposure also has a mild immunomodulatory effect that can reduce the inflammatory component of KP. This isn't an endorsement of unprotected sun exposure — but it does explain why many people notice their smoothest arms during beach season.
The Best Ingredients for KP
Chemical exfoliation is the most effective approach for managing KP. Alpha hydroxy acids (AHAs) like glycolic acid and lactic acid work by dissolving the bonds between dead keratinocytes, helping to clear the follicular plugs that create the bumpy texture. Lactic acid is particularly well-suited for KP because it's both an exfoliant and a humectant — it dissolves keratin while drawing moisture into the skin.
AmLactin Daily Moisturizing Body Lotion contains 12% lactic acid and is one of the most dermatologist-recommended products for KP. The sustained-release formulation provides gentle but effective exfoliation with daily use, gradually smoothing the rough texture over 2–4 weeks of consistent application.
Urea is another powerhouse ingredient for KP. At concentrations of 10–40%, urea acts as both a keratolytic (breaking down excess keratin) and an exceptional humectant. Salicylic acid (a BHA) offers yet another approach — its lipophilic nature allows it to penetrate into the follicle, dissolving the keratin plugs from within. CeraVe SA Cream for Rough & Bumpy Skin combines salicylic acid with ceramides and hyaluronic acid, addressing both exfoliation and barrier repair.
Building an Effective KP Routine
The ideal KP routine balances exfoliation with hydration. Over-exfoliating can cause irritation and paradoxically worsen the rough texture by triggering reactive keratinization. Start with chemical exfoliant application 3–4 times per week and increase to daily use as your skin tolerates it.
In the shower, use a gentle, non-foaming cleanser on affected areas — harsh soaps strip the skin's natural lipids and worsen KP. Avoid harsh physical exfoliants like loofahs, pumice stones, and aggressive body scrubs. While they may temporarily smooth the surface, they cause micro-tears and inflammation that can trigger more keratin production.
After showering, apply your chemical exfoliant treatment to slightly damp skin, then follow with a rich, occlusive moisturizer. Eucerin Roughness Relief Cream combines urea with ceramide-3 and natural moisturizing factors for comprehensive keratolytic and hydrating action. The key is consistency — KP management is a marathon, not a sprint, and results require ongoing maintenance.
What Not to Do
The single most counterproductive thing you can do with KP is pick at, scratch, or squeeze the bumps. Unlike acne, there's nothing inside a KP papule that will 'pop out' — the plug is made of hardened keratin fused to the follicle wall. Picking causes inflammation, potential scarring, and post-inflammatory hyperpigmentation that makes the condition look far worse than the bumps alone.
Avoid hot showers and baths. While they feel soothing, hot water strips the skin's protective lipid barrier and increases transepidermal water loss, worsening the dehydration that exacerbates KP. Use lukewarm water and keep showers short — ideally under 10 minutes.
Don't expect overnight results. KP responds to treatment gradually over weeks, and improvement requires ongoing, consistent care. There is no one-time fix. If you stop your treatment routine, the keratin plugs will reform and the bumps will return. Think of your KP routine like brushing your teeth — it's something you do consistently as part of your daily hygiene, not a temporary treatment.
KP on the Face
While KP most commonly affects the upper arms and thighs, it can also appear on the cheeks — a variant called keratosis pilaris rubra faceii. This facial presentation is particularly common in children and adolescents and manifests as rough, red or pink patches on the cheeks that are often mistaken for rosacea, eczema, or allergic contact dermatitis.
Facial KP requires a gentler treatment approach than body KP because facial skin is thinner and more sensitive. Lower concentrations of chemical exfoliants (5–8% glycolic acid or 5% lactic acid) are appropriate for the face, applied 2–3 times per week rather than daily. Azelaic acid at 10–15% is another excellent option for facial KP — it's keratolytic, anti-inflammatory, and well-tolerated on sensitive skin.
Prescription retinoids (tretinoin, adapalene) are effective for facial KP by normalizing keratinization and promoting cell turnover. However, they should be introduced slowly to avoid irritation. Start with adapalene 0.1% every other night and gradually increase frequency over several weeks.
When KP Might Be Something Else
Several conditions can mimic KP's appearance, and accurate diagnosis ensures appropriate treatment. Follicular eczema can look very similar but involves more inflammation and itching. Fungal folliculitis (pityrosporum folliculitis) presents with uniform small bumps but is caused by yeast overgrowth rather than keratin plugging. Lichen spinulosus causes grouped spiny follicular papules that look like clusters of KP.
If your bumps are painful, pustular, spreading, or associated with other skin changes, see a dermatologist for evaluation. KP is entirely asymptomatic beyond cosmetic texture change — it shouldn't hurt, ooze, or cause significant itching. Any of these additional symptoms suggest a different or concurrent condition.
Children and adolescents with severe KP, particularly in combination with eczema or ichthyosis, should be evaluated by a dermatologist to rule out keratinization disorders that may require more specialized management. These conditions share KP-like features but involve more extensive disruption of the skin's keratinization process.
References
- Thomas M, Khopkar US. "Keratosis pilaris revisited: is it more than just a follicular keratosis?" International Journal of Trichology. 2012;4(4):255-258.
- Poskitt L, et al. "Natural history of keratosis pilaris." British Journal of Dermatology. 1994;130(6):711-713.
- Hwang S, Schwartz RA. "Keratosis pilaris: a common follicular hyperkeratosis." Cutis. 2008;82(3):177-180.