Key Takeaways
- •Perioral dermatitis is a distinct inflammatory condition, not acne or eczema.
- •Topical steroids are the most common trigger and cause — they must be discontinued for healing.
- •The condition predominantly affects women aged 20-45.
- •Treatment requires a minimalist skincare approach and often oral antibiotics.
- •Steroid withdrawal can cause a temporary flare that feels worse before it gets better.
- •Heavy cosmetics, fluorinated toothpaste, and SLS-containing products can trigger flares.
What Perioral Dermatitis Looks Like
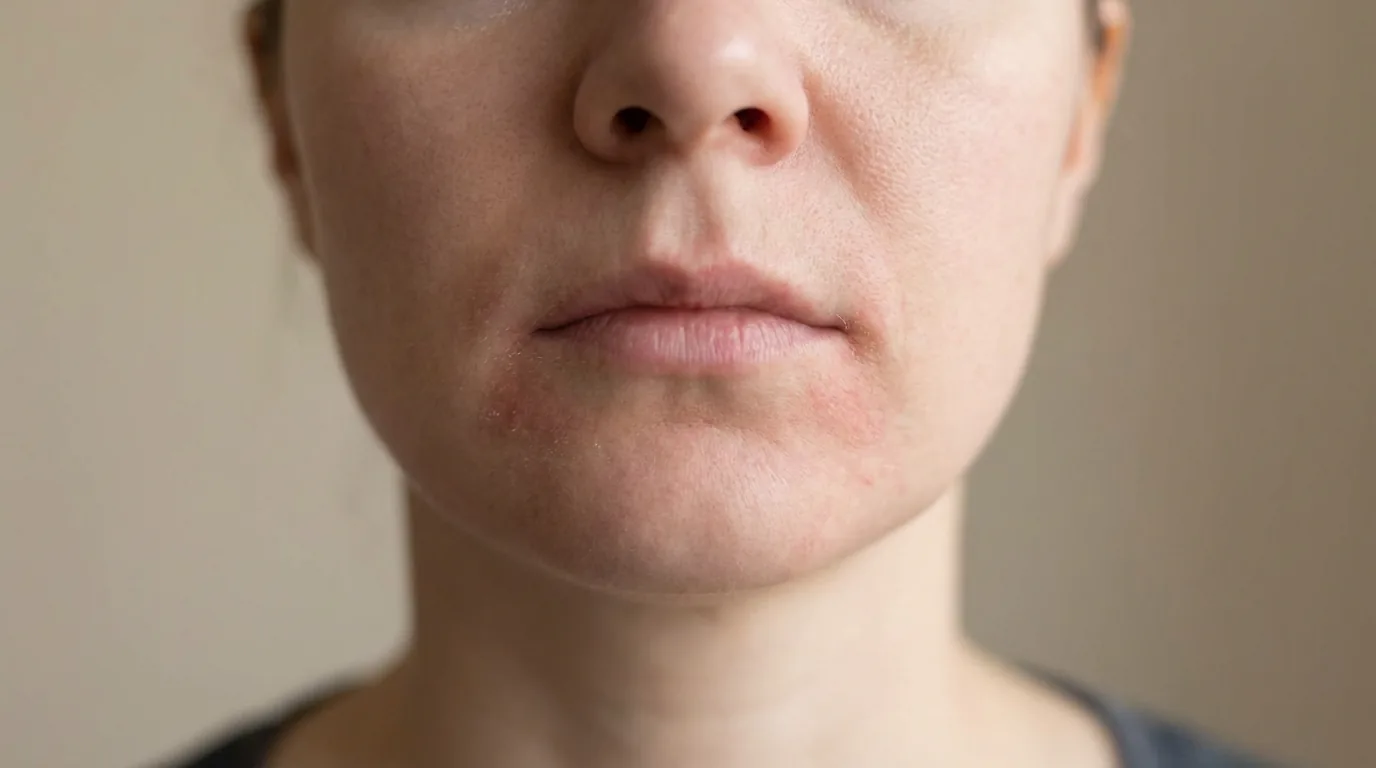
Perioral dermatitis presents as clusters of small, red, inflamed papules and pustules concentrated around the mouth — particularly in the nasolabial folds and on the chin. A characteristic feature is the sparing of the vermillion border: there's typically a clear zone of normal skin immediately adjacent to the lip line, with the rash beginning 2-3mm away. This clear border helps distinguish perioral dermatitis from other conditions like contact dermatitis or herpes simplex.
Despite its name, perioral dermatitis doesn't always confine itself to the perioral area. It frequently extends to the perinasal region (around the nostrils) and can involve the periocular area (around the eyes). When it involves these additional areas, it's sometimes called periorificial dermatitis. The rash can be mildly itchy or have a burning sensation, but severe itching is uncommon.
The condition predominantly affects women between ages 20 and 45, though it can occur in men, children, and older adults. In children, the perinasal and periocular distributions are more common than the classic perioral pattern. The condition is chronic and relapsing — without appropriate treatment, it can persist for months or years.
Common Triggers and Causes
The most well-established trigger for perioral dermatitis is topical corticosteroid use. The relationship is insidious: a patient develops a rash, applies a steroid cream, the rash temporarily improves, but when the steroid is discontinued, the rash rebounds worse than before. This leads to increasing reliance on steroids, creating a vicious cycle of application, improvement, withdrawal, and worsening.
Inhaled corticosteroids for asthma can also trigger perioral and perinasal dermatitis, particularly if the inhaler spray contacts the skin around the mouth and nose. Nasal steroid sprays can similarly contribute to perinasal presentations. Even 'mild' over-the-counter hydrocortisone used repeatedly on the face can initiate the cycle.
Other triggers include heavy cosmetic creams and foundations (particularly those containing petrolatum or paraffin), fluorinated toothpaste, sodium lauryl sulfate in oral care products, and physical factors like excessive face washing, wind exposure, and UV radiation. Hormonal fluctuations, particularly around menstruation, can exacerbate the condition. Some research suggests a role for Demodex mites and Candida organisms in the pathogenesis.
Why It's Not Acne
Perioral dermatitis is frequently misdiagnosed as acne, leading to inappropriate treatment that often worsens the condition. While both conditions feature papules and pustules, there are key distinguishing features. Perioral dermatitis lacks comedones (blackheads and whiteheads) — these are a hallmark of acne vulgaris but are absent in perioral dermatitis.
The distribution is also different. Acne typically affects the T-zone, cheeks, and jawline in a scattered pattern. Perioral dermatitis concentrates around the mouth, nose, and eyes in a more defined, grouped pattern. The texture of perioral dermatitis lesions is finer and more granular than typical acne papules, and the surrounding skin often has a dry, scaly quality that's atypical for acne.
This distinction matters because many acne treatments worsen perioral dermatitis. Benzoyl peroxide, strong retinoids, and aggressive exfoliating acids can all irritate the compromised skin and exacerbate the rash. The minimalist approach required for perioral dermatitis is the opposite of the multi-active regimen typically used for acne.
The Steroid Withdrawal Phase
If topical steroids are identified as the trigger, discontinuing them is essential — but this comes with an uncomfortable reality known as steroid withdrawal or rebound dermatitis. When the steroid is stopped, the suppressed inflammation rebounds, often making the rash significantly worse before it improves. This flare can be intense and lasts anywhere from several days to several weeks.
The severity of the withdrawal flare generally correlates with the potency and duration of steroid use. Someone who used mild hydrocortisone for a few weeks will likely experience a milder rebound than someone who used a potent fluorinated steroid for months. Abrupt discontinuation of potent steroids may require a gradual taper to manage the withdrawal, transitioning to a lower-potency steroid before stopping entirely.
During the withdrawal phase, patients need significant emotional support and reassurance. The worsening rash can be distressing and creates a powerful urge to reapply the steroid. Understanding that this is a temporary, expected phase of healing — not a sign that the steroid is needed — is crucial for successful treatment.
Evidence-Based Treatment
The first-line treatment for perioral dermatitis is oral antibiotics, with doxycycline being the most commonly prescribed. The therapeutic effect is thought to be anti-inflammatory rather than antimicrobial — low-dose doxycycline (40mg modified-release daily) can be effective while minimizing antibiotic-related side effects. A typical course lasts 6–12 weeks, with improvement usually visible within 2–3 weeks.
Topical treatments that have shown efficacy include metronidazole 0.75–1% cream or gel, applied twice daily. Azelaic acid (15–20%) is another effective option with anti-inflammatory and antimicrobial properties. Pimecrolimus 1% cream (a calcineurin inhibitor) can be used as a steroid-free anti-inflammatory, though some data suggests it may occasionally trigger perioral dermatitis in susceptible individuals.
Topical ivermectin 1% cream, originally developed for rosacea, has shown promising results for perioral dermatitis, particularly in cases where Demodex mites may be contributing. This is an off-label use, but the anti-parasitic and anti-inflammatory properties make it a logical option when first-line treatments are insufficient.
Skincare During Treatment and Recovery
The guiding principle during perioral dermatitis treatment is radical simplification. Strip your routine down to the bare essentials: a gentle cleanser, a simple moisturizer, and sunscreen. Nothing else. No actives, no serums, no masks, no toners. The compromised skin barrier in perioral dermatitis makes it hypersensitive to ingredients that would normally be well-tolerated.
Vanicream Gentle Facial Cleanser is an excellent choice during treatment — it's free of dyes, fragrance, masking fragrance, lanolin, parabens, and formaldehyde releasers. For moisturizing, Avène Tolerance Extrême Emulsion contains only seven ingredients and is designed for hypersensitive, reactive skin. Its sterile packaging prevents contamination that could further irritate compromised skin.
La Roche-Posay Toleriane Double Repair Face Moisturizer is another well-tolerated option that provides ceramide-based barrier repair. When selecting sunscreen, opt for mineral formulations (zinc oxide, titanium dioxide) as chemical sunscreen filters can irritate perioral dermatitis. Avoid applying sunscreen directly to actively inflamed areas if it causes stinging.
Preventing Recurrence
Perioral dermatitis can recur, particularly if underlying triggers aren't identified and eliminated. The most important preventive measure is avoiding topical steroids on the face entirely. If you need anti-inflammatory treatment for another facial condition, discuss non-steroidal alternatives with your dermatologist.
Switch to fluoride-free toothpaste and SLS-free oral care products, as these are recognized triggers. Avoid heavy, occlusive facial cosmetics, especially around the mouth and nose. When reintroducing skincare products after recovery, do so one at a time with at least a week between additions to identify any that trigger recurrence.
If you use an inhaled corticosteroid for asthma, use a spacer device and rinse your mouth and face after each use to minimize skin contact. For patients with recurrent perioral dermatitis, maintenance therapy with low-dose doxycycline or intermittent topical metronidazole may be recommended to prevent flares.
References
- Lipozencic J, Ljubojevic S. "Perioral dermatitis." Clinics in Dermatology. 2011;29(2):157-161.
- Wollenberg A, et al. "Perioral dermatitis." Journal of the German Society of Dermatology. 2011;9(5):422-428.
- Hafeez ZH. "Perioral dermatitis: an update." International Journal of Dermatology. 2003;42(7):514-517.
- Malik R, Quirk CJ. "Topical applications and perioral dermatitis." Australasian Journal of Dermatology. 2000;41(1):34-38.